Do you suffer from urticaria (hives)?
- Definition
- Classification
- Treatment
Definition
Urticaria is a very common problem:
One person in five will suffer from it during the course of their life (at differing times). Sometimes, it represents a true allergic reaction caused by a food, an animal, a medication, an insect sting, a chemical product or other sensitizing agent such as latex. However, most often, urticaria is not allergic in nature. Therefore, you mustn't be surprised if the allergist suggests not to do any allergy testing.
Classically urticaria is characterised by itchy swollen areas of many different sizes on the skin. The lesions are fleeting and don't leave a trace: the skin is not "sick". There is no subsequent desquamation, unlike in contact dermatitis ("allergic"). When urticaria involves deeper tissues, one speaks of "angioedema".
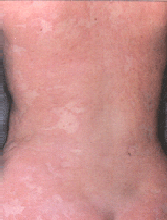
Urticaria or hives
Classification of urticaria
The principal antigens capable of producing allergic asthma are the seasonal allergens (tree pollen, grass pollen, ragweed and certain seasonal molds) and the permanent allergens (skin of furry animals, dust mites, and certain interior molds).
1) "Allergic" urticaria
Other than certain reactions to medication, the allergic cause of urticaria is easily recognized by the afflicted individual. In general, urticaria follows less than 30 minutes after ingestion of contact with the sensitizing agent (food, insect, etc.). Skin tests can be very useful in confirming the diagnosis of allergy.
2) "Non allergic" urticaria
a) Physical urticaria
Diverse physical stimuli (heat, exercise, the sun, cold, pressure and vibration) may provoke urticaria. This kind of urticaria is called "physical", and very often occurs rapidly (several minutes) after a physical stimulus, except in certain cases of pressure urticaria which can occur later.
Late-onset pressure urticaria (belt, bras, hands of a manual labourer, etc.) is particular, because it is often chronic, difficult to treat and characterized by lesions that are warm rather than itchy. This "inflammatory" urticaria may also be precipitated by the ingestion of "irritant" foods.
b) "Pseudo-allergic" urticaria

Urticaria, another example
Several substance labelled as "non-specific histamine liberators" (foods, hormones, medications, etc.) can provoke urticaria. Among these agents, the classics are: codeine, morphine, several antibiotics, radio-contrast products used in radiology, the curares (general anaesthesia) and dextran. Finally, numerous foods (strawberries, fermented products, honey, etc.) in addition to aspirin (ASA) and other anti-inflammatories can provoke a "pseudo-allergic" urticaria, quite rapidly in predisposed subjects. Unfortunately, in all these cases, allergy tests are unreliable.
c) "Secondary" urticaria
Sometimes, urticaria is associated with an auto-immune disease, a hypocomplementemia, thyroid disease, cancer, or an infection (parasites, helicobacter pylori, etc.). Obviously, these pathologies need to be eliminated.
d) "Reflex" urticaria
Recent studies of several hormones (gastrin, neurohormones) suggest that there is a link between these substances, mastocytes and the skin. It seems, therefore, that several "external irritants" (emotional, food, etc.) could cause urticaria (that is often called "idiopathic").
e) Hereditary angioneurotic angioedema and acquired deficiencies in the inhibitor of C1 esterase . These very rare conditions are associated with a non-itchy angioedema in particular that may also manifest internally (within the intestines, etc.).

Dermographism
Treatment of urticaria
1) Eliminate the allergic cause (food, medication, contact allergen, etc.). In the same way for "pseudo-allergic" urticaria, eliminate the provoking agent.
2) Avoid factors that evoke the physical urticarias, such as excessive heat, the sun, tight clothing or irritants,etc. Also avoid vasodilatory factors which may potentialise urticaria, such as alcohol, nicotinic acid, anti-inflammatories, several anti-hypertensive medications and diverse food "irritants" (acidic foods, spices, fermented foods, charcuterie, and many exotic dishes).
3) Treat, if possible, any disease which may be the cause of the urticaria (secondary urticaria or angioedema).
4) Pharmacotherapy: above-all "symptomatic" (anti-histamines), with new non-sedating agents with long half-lives (cetirizine, loratadine, desloratadine, fexofenadine).
Sometimes, a more powerful antihistamine may be necessary, or in association with an "anti-H2" (such as ranitidine). Certain cases of physical or cold urticaria respond better to agents such as cyproheptadine or doxepine.
In the case of treatment failure with conventional medication, the allergist may prescribe corticosteroids or other less "classic" medications.
__________________________
 The Association of Allergists and Immunologists of Québec
The Association of Allergists and Immunologists of Québec